3M ESPE Filtek P60 Posterior Restorative
- Brand: 3M ESPE
-
( 8 Reviews )Rated 4.50 out of 5 based on 8 customer ratings08
US$35.00US$55.00 (-36%)

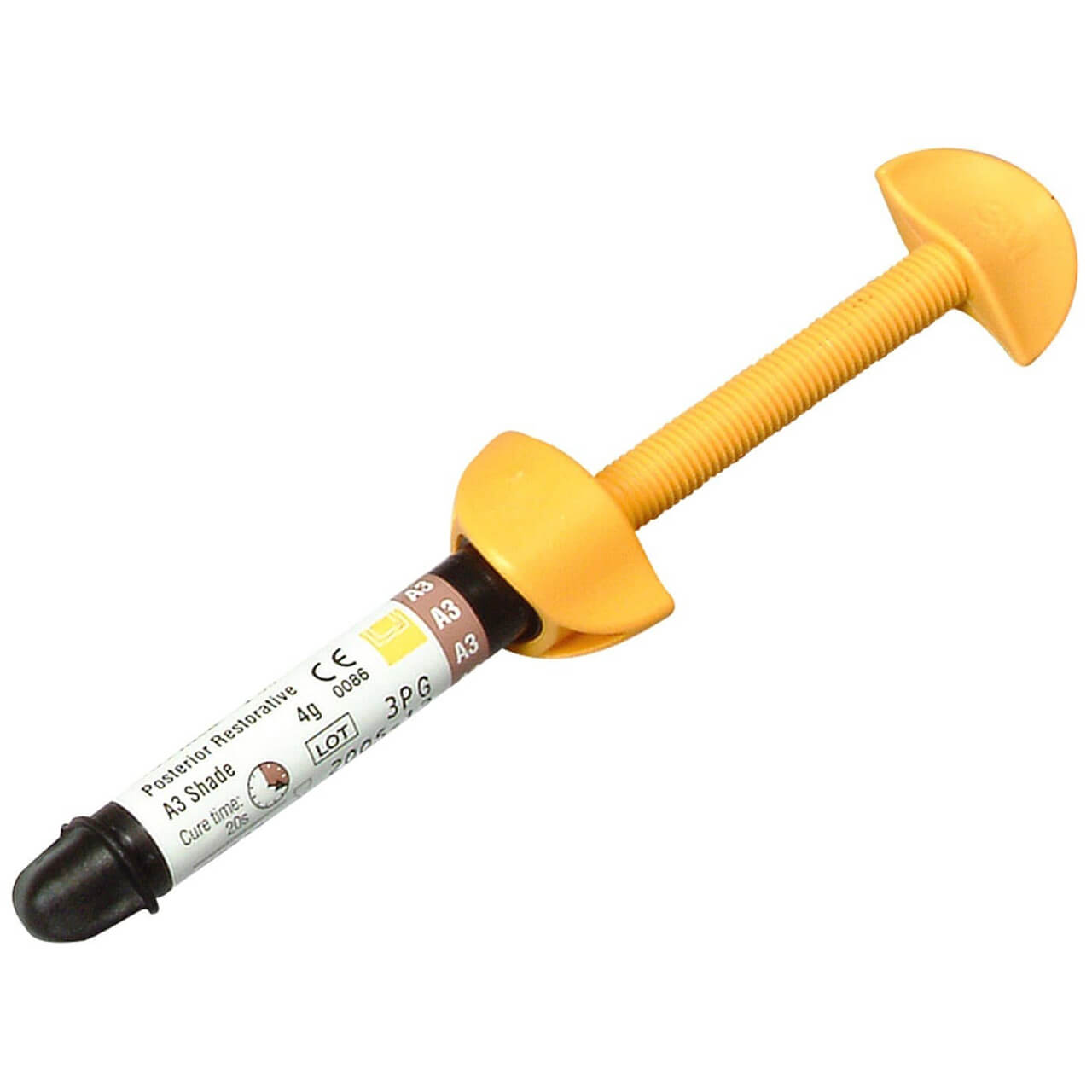
3M ESPE P60 Micro Hybrid Posterior Syringe Original
Made In USA
3M ESPE Filtek P60 Posterior Restorative, is a visible-light activated, radiopaque, restorative composite. It is designed for use in posterior restorations. The filler in Filtek P60 restorative is zirconia/silica. The inorganic filler loading is 61% by volume (without silane treatment) with a particle size range of 0.01 to 3.5 μm. Filtek P60 restorative contains BIS-GMA, UDMA, and BIS-EMA resins. A dental adhesive is used to permanently bond the restoration to the tooth structure. The restorative is available in a variety of shades. It is packaged in traditional syringes
FEATURES :-
- Available in three shades
- Superior packability
- Fast curing-time – only 20 seconds to cure an increment of 2.5mm
- Excellent strength
- Wear resistance
- Low polymerisation shrinkage
Superior Packability :
- Packs well without sticking to instrument. Excellent marginal adaptation and interproximal contact
Easy Sculpting :
- With exceptional resistance to slumping
Fastest Placement Technique:
- Takes only 20 seconds to cure an increment of 2.5mm
Low Polymerization Shrinkage:
- Less stress on the tooth, less sensitivity potential for the patient
Excellent Wear Resistance and Strength
- Means you can be confident of long-lasting posterior restorations.
INDICATIONS :-
- Direct posterior restorations class I and II
- Sandwich technique with glass ionomer resin material
- Cusp buildups
- Core buildups
- Splinting
- Indirect posterior restorations including inlays and onlays
Instructions for Use :-
Preparation
1. Prophy: Teeth should be cleaned with pumice and water to remove surface stains
2. Shade Selection: Before isolating the tooth, select the appropriate shade(s) of restorative material using the Filtek P60 shade guide
3. Isolation: A rubber dam is the preferred method of isolation. Cotton rolls plus an evacuator can also be used.
Directions for DIRECT RESTORATIONS
1. Cavity Preparation: Prepare the cavity. Line and point angles should be rounded. No residual amalgam or other base material should be left in the internal form of the preparation that would interfere with light transmission and therefore, the hardening of the restorative material.
2. Pulp Protection: If a pulp exposure has occurred and if the situation warrants a direct pulp capping procedure, use a minimum amount of calcium hydroxide on the exposure followed by an application of Vitrebond™ or Vitrebond™ Plus Light Cure Glass lonomer Liner/Base, manufactured by 3M ESPE. Vitrebond liner/bases may also be used to line areas of deep cavity excavation. See Vitrebond liner/base instructions for details
3. Placement of Matrix: Place a thin dead-soft metal, or a precontoured-Mylar or a precontoured-metal matrix band and insert wedges firmly. Burnish the matrix band to establish proximal contour and contact area. Adapt the band to seal the gingival area to avoid overhangs. Note: The matrix may be placed following the enamel etching and adhesive application steps if preferred
4. Adhesive System: Follow the manufacturer’s instructions regarding etching, priming, adhesive application and curing
5. Dispensing the Composite: Dispense the necessary amount of restorative material from the syringe onto the mix pad by turning the handle slowly in a clockwise manner. To prevent oozing of the restorative material when dispensing is completed, turn the handle counterclockwise a half turn to stop paste flow. Immediately replace syringe cap. If not used immediately, the dispensed material should be protected from light.
6. Placement:
6.1 Place and light cure restorative in increments no thicker than 2.5 mm
6.2 Slightly overfill the cavity to permit extension of composite beyond cavity margins. Contour and shape with appropriate composite instruments
6.3 Avoid intense light in the working field
6.4 Posterior placement hints: a) To aid in adaptation, the first 1 mm layer may be placed and adapted to the proximal box. b) A condensing instrument (or similar device) can be used to adapt the material to all of the internal cavity aspects
7. Curing: This product is intended to be cured by exposure to a halogen or LED light with a minimum intensity of 400mW/cm2 in the 400-500 nm range. Cure each increment by exposing its entire surface to a high intensity visible light source, such as 3M ESPE curing light for 20 seconds. Hold the light guide tip as close to the restorative as possible during light exposure
8. Finishing: Contour restoration surfaces with fine finishing diamonds, burs or stones. Contour proximal surfaces with Sof-Lex™ Finishing Strips, manufactured for 3M ESPE
9. Adjust Occlusion: Check occlusion with a thin articulating paper. Examine centric and lateral excursion contacts. Carefully adjust occlusion by removing material with a fine polishing diamond or stone
10. Polishing: Polish with Sof-Lex Finishing and Polishing System and with white stones or rubber points where discs are not suitable
Directions for Indirect Procedure
For Inlays, Onlays Or Veneers
1. Dental Operatory
Procedure
1.1 Shade selection: Choose the appropriate shade(s) of Filtek P60 restorative prior to isolation. If the restoration is of sufficient depth, use of an opaque shade is recommended
1.2 Preparation: Prepare the tooth
1.3 Impressioning: After preparation is complete, make an impression of the prepared tooth by following the manufacturer’s instructions of the impressioning material chosen. An impressioning material, such as manufactured by 3M ESPE, may be used.
2. Laboratory Procedure
2.1 Pour the impression of the preparation with die stone. Place pins at the preparation site at this time if a “triple tray” type of impression was used
2.2 Separate the cast from the impression after 45 to 60 minutes. Place pins in die and base the cast as for a typical crown and bridge procedure. Mount or articulate the cast to its counter model to an adequate articulator
2.3 If a second impression was not sent, pour a second cast using the same impression registration. This is to be used as a working cast
2.4 Section out the preparation with a laboratory saw and trim away excess or, expose the margins so they can be easily worked. Mark the margins with a red pencil if needed. Add a spacer at this time if one is being used
2.5 Soak the die in water, then with a brush, apply a very thin coat of separating medium to the preparation, let it dry somewhat, then add another thin layer
2.6 Add the first third of composite to the floor of the preparation, stay short of the margins, light cure for 20 seconds
2.7 Add the second third of composite. Allow for the last third (incisal) to include the contact areas, light cure for 20 seconds
2.8 Place the die back into the articulated arch, add the last third of composite to the occlusal surface. Overfill very slightly mesially, distally, and occlusally. This will allow for the mesiodistal contacts and the proper occlusal contact when the opposing arch is brought into occlusion with the uncured incisal increment. Light cure for only ten seconds, then remove the die to prevent adhering to adjacent surfaces. Finish the curing process
2.9 With the occlusal contacts already established, begin removing the excess composite from around the points of contact. Develop the inclines and ridges as per remaining occlusal anatomy
2.10 Care must be taken when removing the prosthesis from the die. Break off small amounts of the die from around the restoration, the die stone should breakaway cleanly from the cured restoration, until all of the restoration is recovered
2.11 Using the master die, check the restoration for flash, undercuts, and fit. Adjust as necessary, then polish.
3. Dental Operatory Procedure
3.1 Roughen the interior surfaces of the indirect restoration.
3.2 Cementation: Cement the prosthesis using a 3M ESPE resin cement system by following manufacturer’s instructions.
Additional information
| Shade | A3, B2, C2 |
|---|
Average Rating
4.50
Only logged in customers who have purchased this product may leave a review.












by Chakor
Superior packability
by emidio
Superior packability.Excellent strength.Wear resistance
by baibin
Excellent strength.Wear resistance.Low polymerisation shrinkage